Despite high biocompatibility of titanium and its alloys, this metal causes various side effects in the human body. It is believed that titanium biomaterials may induce an innate/adaptive immune response. However, still little is known about changes caused by titanium mandible implants, particularly with regard to bone healing.
Tag Archives: Titanium and Peri-Implantitis
Dental implants are often made of titanium alloys. Implant therapy currently promises a good long-term result without impacting health; however, its success depends on many factors. In this article, the authors focus on the most common risk factors associated with metallic surgical implants.
Metallic implants placed in humans exhibit wear and corrosion that result in the liberation of metal-containing by-products. In the case of titanium (Ti) containing implants, the metal containing debris may exist in a number of states, including metallic particles produced by mechanical wear and the products of metal corrosion in biological environments, such as the joints and surrounding fluids and tissues.
Titanium implants are routinely used for bone fractures as well as dental work. It has recently been shown that titanium-based implants both corrode and degrade, generating metallic debris. There is some concern over the increased concentrations of circulating metal-degradation products derived from these implants, and their potential harmful biological effects over a period of time, including hepatic injury and renal lesions.
This review is based on current titanium research demonstrating the many factors that can pose a negative impact on human health when exposed to the various forms of titanium, including its relationship and interactions with other metals.
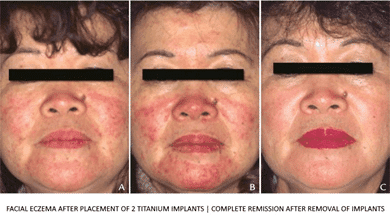
This review of the literature indicates that titanium can induce hypersensitivity in susceptible patients and could play a critical role in implant failure.
This study indicates that titanium is unsuitable as a biomaterial in devices which are in direct contact with blood for a prolonged period.
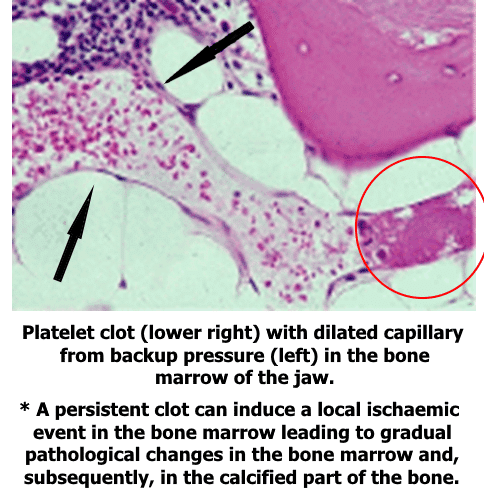
Ischaemic hypoxic medullary bone occurs when there is a disruption in the vascular supply of that bone tissue. Such disruption can occur when a thrombus (clot) is formed and does not subsequently break down (fibrinolysis).
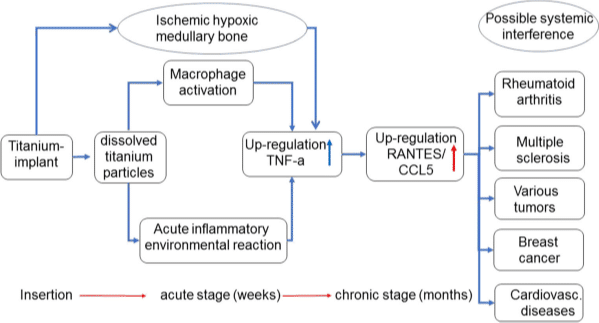
All DTI (Dental Titanium Implant)-FDOJ (Fatty Degeneration with Osteonecrosis of the Jaw) samples showed RANTES/CCL5 (R/C) as the only extremely overexpressed cytokine. DTI-FDOJ cohort showed a 30-fold mean overexpression of R/C as compared with a control cohort of 19 healthy JB samples.
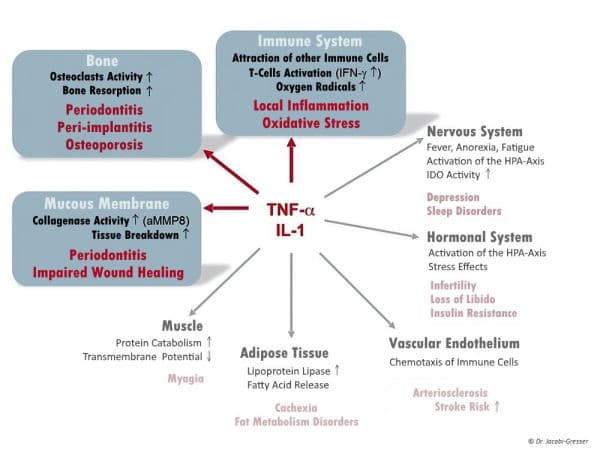
Peri-implantitis is a pathogenetically complex clinical picture and, in addition to local effects, has systemic effects depending on individual genetic susceptibility. It has some similarities to periodontitis but differs in the taxonomic biofilm composition and is also involved in foreign body reactions to the implant material.
- 1
- 2