Conclusion
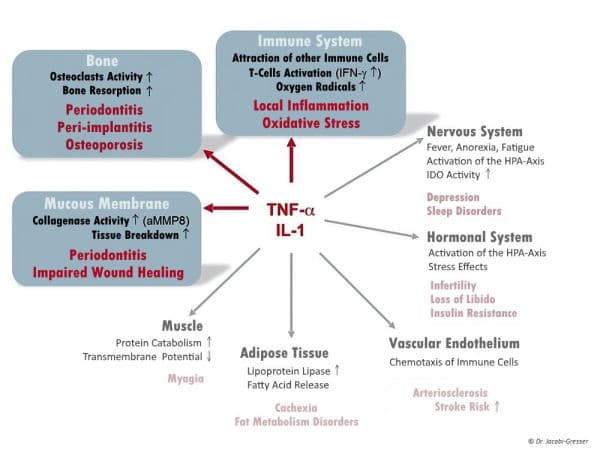
Peri-implantitis is a pathogenetically complex clinical picture and, in addition to local effects, has systemic effects depending on individual genetic susceptibility. It has some similarities to periodontitis but differs in the taxonomic biofilm composition and is also involved in foreign body reactions to the implant material. Patients with a periodontitis history have a genetically higher risk of developing peri-implantitis. Pre-implantological risk diagnostics for appropriately scheduled patients allows for a differentiated implant-prosthetic procedure with the aim of avoiding peri-implantitis development. For early diagnosis and therapy monitoring, laboratory biomarkers such as calprotectin or the aMMP-8 determination from the sulcus fluid are now available to initiate anti-inflammatory measures at an early stage and to control their efficiency. An adapted to the patient monitoring in defined time intervals is indispensable due to individual risk burdening.